Sometimes, it helps to know a guy.
Especially one who has the inside scoop.
Mary Gryzwa, who is in her 70s, had low back pain that worsened in 2015. She was diagnosed with spinal stenosis, a narrowing of the spinal canal which puts pressure on nerves and causes pain.
“I had excruciating pain and couldn’t do anything like I wanted to, like walking and biking and playing golf,” she says.
The back pain interfered with Mary’s sleep, too. “Oh, I was up all night walking the floor,” she says.
Mary tried physical therapy, injections, ultrasound and acupuncture, but had gotten “not one bit, not one iota” of relief from her back pain, she says.
“It just got worse and worse and worse,” says Mary, who lives in Peshtigo, Wisconsin.
“And then my son says, ‘I think we can help you, Mom,’ and they did.”
Mary’s son, Mark, is an engineer with a medical technology company. He suggested she consider a pain management product – a spinal cord stimulator, or neurostimulator – for which a new version was being rolled out.
The device uses tiny amounts of electricity to stimulate areas of the spine to suppress pain signals from the low back to the brain. It’s controlled by a hand-held remote that’s about the size of a cellphone.
A spinal cord stimulator is typically implanted under the skin in the lower back. It’s small and thin, about the size of an Oreo cookie. Some people have it implanted in the buttocks to keep it hidden under clothes.
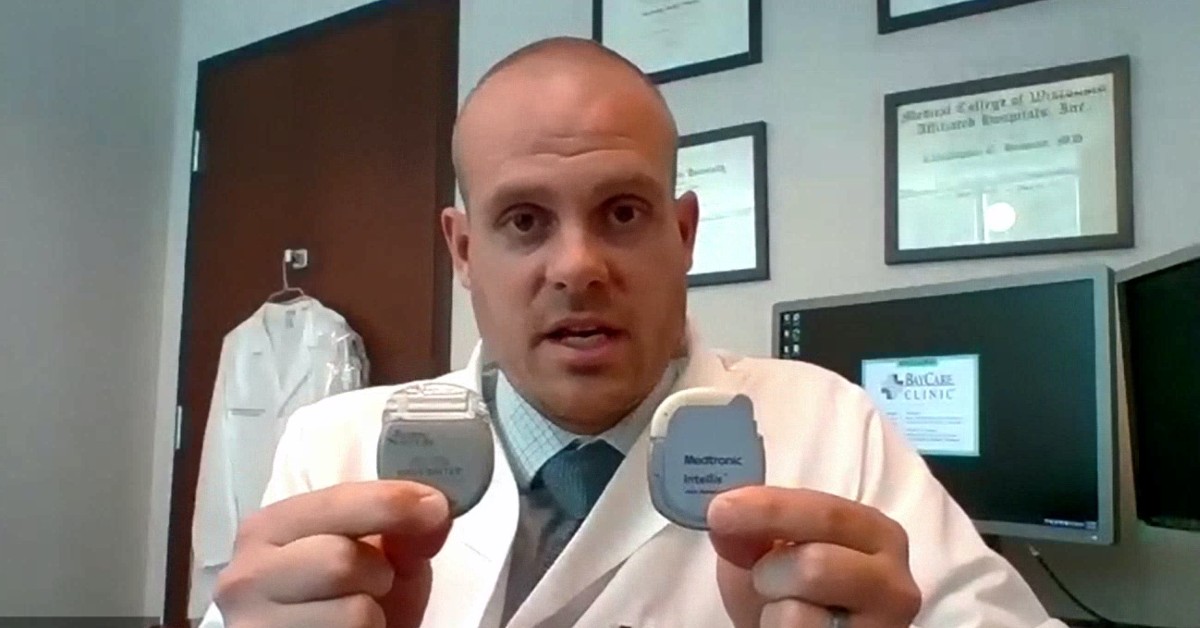
Mary turned to Dr. Christopher Howson, a fellowship-trained pain medicine physician with BayCare Clinic Pain & Rehab Medicine. He embraced the idea.
It helps to know a guy like that, too.
“When she came to me, she already had that sort of in mind as a possibility for treatment when some of the other stuff wasn’t working,” Howson says.
Mary became the first person in Wisconsin to use the newest model of this pain management technology.
The new version of the spinal cord stimulator became available in September 2017. Howson examined Mary and recommended it to her in October. Mary tried it for 12 days in November, during which the neurostimulator was taped to her torso. That went well.
Three weeks later, in December 2017, Howson implanted the spinal cord stimulator into Mary’s lower back. That was outpatient surgery at Aurora BayCare Medical Center in Green Bay.
And now?
“It’s phenomenal. It’s very successful treating my pain. Now I am able to do bike riding and walking and golfing like I used to,” Mary says. “And I can also sleep better at night.”
The spinal cord stimulator’s settings can be adjusted to treat varying levels of pain – most often by phone with the help of support staff – and its software can be upgraded as pain management technology evolves. After Mary’s neurostimulator software was upgraded in June 2020, she experienced improved pain relief.
“It is amazing,” Mary says. She expects to use the spinal cord stimulator for the rest of her life.
Good candidates for a spinal cord stimulator have low back pain, leg pain or a combination of the two, Howson says. The device is occasionally used to treat pain in the upper extremities.
“I would tell anybody to go forward with it because it really does help,” Mary says.
She’s happy, and so is Howson.
“It’s the cool part about my job,” Howson says of Mary and patients like her. “They’re very normal people. They just want to go to the grocery store. They want to hang out with their grandchildren. They want to play a round of golf. … They have very reasonable expectations, and because of some of the pain they have, they can’t do those. To be able to give them tools to do that is a great part of my job.”
